For this posting I would like to talk about some of the pedagogy around simulation. The vision for our simulation suites is that they will be used to get at more of the nebulous parts of being a nurse; those things that we cannot really address anywhere but in the moment. Things like critical thinking, collaboration, interprofessional team work and conflict management are some examples of these hard to recreate situations. Now that we have these simulation suites that are set up to recreate the clinical setting as realistically as possible, we can also recreate some of these sticky situations as realistically as possible and allow the students the time and space to work through them without patient care or safety being put in jeopardy.
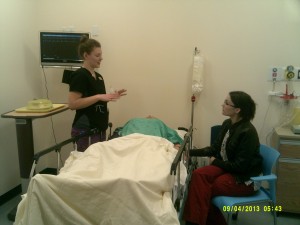 My particular area of interest revolves around the interdisciplinary possibilities. As we have three programs using these suites (Registered Nurse (RN), Licensed Practical Nurse (LPN) and Health Care Aide (HCA)), the possibilities are exciting. For example, one of the scenarios I want to work on soon is one that is encountered all too often in the clinical area. An LPN may have a patient assignment that is appropriate for his/her scope, but the patient takes a turn for the worse and becomes too acute (read sick) and now requires too many interventions and assessments that fall outside of LPN’s scope. At this point, the RN working with the LPN should take over care of this patient, and the RN and LPN negotiate what the LPN might take over from the RN to even the load a bit. What happens all too often is that either a) the LPN does not realize that the patient should become an RN assignment or b) the RN declines taking on the care of this patient for whatever reason. Neither of these should happen, but they do. The beauty of designing a simulation around these two roads leading to the same outcome (potential conflict) is that I can design the simulation from either perspective since either RN or LPN learners may be involved. If I have LPN learners, I can design it so the RN refuses to take on the care of the now sicker patient. If I have an RN learner, I can have the LPN not pick up on the cues that this patient is now moving to the edge of his/her scope. If I have both an RN and LPN learner (bliss!) we can do the scenario both ways and see how it differs for them each time.
My particular area of interest revolves around the interdisciplinary possibilities. As we have three programs using these suites (Registered Nurse (RN), Licensed Practical Nurse (LPN) and Health Care Aide (HCA)), the possibilities are exciting. For example, one of the scenarios I want to work on soon is one that is encountered all too often in the clinical area. An LPN may have a patient assignment that is appropriate for his/her scope, but the patient takes a turn for the worse and becomes too acute (read sick) and now requires too many interventions and assessments that fall outside of LPN’s scope. At this point, the RN working with the LPN should take over care of this patient, and the RN and LPN negotiate what the LPN might take over from the RN to even the load a bit. What happens all too often is that either a) the LPN does not realize that the patient should become an RN assignment or b) the RN declines taking on the care of this patient for whatever reason. Neither of these should happen, but they do. The beauty of designing a simulation around these two roads leading to the same outcome (potential conflict) is that I can design the simulation from either perspective since either RN or LPN learners may be involved. If I have LPN learners, I can design it so the RN refuses to take on the care of the now sicker patient. If I have an RN learner, I can have the LPN not pick up on the cues that this patient is now moving to the edge of his/her scope. If I have both an RN and LPN learner (bliss!) we can do the scenario both ways and see how it differs for them each time.
 I spoke last time of the complex simulations we had both purchased and made and finding a place for these complex scenarios can be a challenge. The literature suggests that the best scenarios should be no longer than 20 minutes with 15 to 20 minutes of debriefing. The majority of the learning and certainly the deep learning should come from the reflection associated with the debriefing. This means that if a simulation is too long, the learner simply will not have time or memory enough to recall all that went on during a longer scenario. Certainly not enough for getting at the assumptions and data that went into decisions and priority setting. So the question becomes how to chop these longer, more complex scenarios into more manageable chunks? One of the things that we will be trying in coming weeks is to tag team the learning. Learners will play nurses coming on and going off shift or off to a meal break and handing their patient to another learner playing the nurse coming on duty or covering them for their breaks. I have tried to chunk particular learning into each segment, whether it be learning around assessments, dealing with a complication, or priority setting in completing skills like medication administration and catheter insertion. We shall see how this goes. Next posting, I will discuss the art and science of debriefing in more detail.
I spoke last time of the complex simulations we had both purchased and made and finding a place for these complex scenarios can be a challenge. The literature suggests that the best scenarios should be no longer than 20 minutes with 15 to 20 minutes of debriefing. The majority of the learning and certainly the deep learning should come from the reflection associated with the debriefing. This means that if a simulation is too long, the learner simply will not have time or memory enough to recall all that went on during a longer scenario. Certainly not enough for getting at the assumptions and data that went into decisions and priority setting. So the question becomes how to chop these longer, more complex scenarios into more manageable chunks? One of the things that we will be trying in coming weeks is to tag team the learning. Learners will play nurses coming on and going off shift or off to a meal break and handing their patient to another learner playing the nurse coming on duty or covering them for their breaks. I have tried to chunk particular learning into each segment, whether it be learning around assessments, dealing with a complication, or priority setting in completing skills like medication administration and catheter insertion. We shall see how this goes. Next posting, I will discuss the art and science of debriefing in more detail.